To use all functions of this page, please activate cookies in your browser.
my.chemeurope.com
With an accout for my.chemeurope.com you can always see everything at a glance – and you can configure your own website and individual newsletter.
- My watch list
- My saved searches
- My saved topics
- My newsletter
Kleihauer-Betke testThe Kleihauer-Betke ("KB") test, Kleihauer-Betke ("KB") stain or Kleihauer test, is a blood test used to measure the amount of fetal hemoglobin transferred from a fetus to an Rh-negative mother's bloodstream.[1] The results of the test are used to determine the required dose of Rh immune globulin (RhIg) to inhibit formation of Rh antibodies in the mother and prevent Rh disease in future Rh-positive children. In this test, hemoglobin is eluted from the mother's red blood cells, whereas the fetal hemoglobin is resistant to this acid elution. When the slides are stained, the maternal cells appear very pale, whereas fetal cells are stained and appear bright pink. Simple comparative counts allow an estimate of whether a significant fetal-maternal hemorrhage has occurred. In those with positive tests (25% or more of estimated fetal blood volume lost), follow up testing (at a postpartum check) should be done to rule out the possibility of a false positive because of a process, such as e.g. sickle cell trait, in the mother which causes persistent elevation of fetal hemoglobin. The KB test is the standard method of detecting fetal-maternal hemorrhage (FMH). This takes advantage of the differential resistance of fetal hemoglobin to acid. A standard blood smear is prepared from the mother's blood. An acid bath is then used to remove all adult hemoglobin but does not remove fetal hemoglobin. Subsequent staining makes fetal cells (containing fetal hemoglobin) appear rose-pink in color, while adult cells are only seen as 'ghosts'. A large number Comparison with other more expensive or technologically advanced methods such as flow cytometry has shown that the KB stain, like the more advanced methods, is sensitive in its detection of FMH.[1] Background counting errors can result in estimates of as much as 5 ml fetal blood loss when there actually is no such blood loss, but standard methods available in most laboratories admit an extremely low probability of the return of a false positive when more severe FMH has taken place. Product highlight
Estimating the Severity of FMHTo determine if a positive test for FMH should be considered as the likely cause of fetal death, the percent of total fetal blood volume lost should be calculated, making appropriate adjustments based on the following known relationships:
These constraints can then be applied to yield the formula 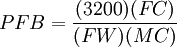 where
An Example of How This Formula is Used in Resolving a StillbirthSuppose that a KB stain is performed and TC = 5000 total red blood cells are observed, FC = 200 of which are found to be fetal red blood cells. Suppose further that the stillbirth weight of the fetus under consideration is FW = 2.0kg. Then we would conclude that the total percentage of fetal blood lost is approximately 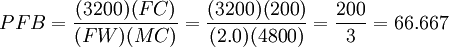 to five significant digits. We would hence conclude that the fetus under consideration lost 66.667% (two thirds) of its blood via FMH. Generally, stillbirth is highly probable for any value of Problems in the Detection of Fetal Red Blood CellsSince fetal and maternal blood cells have the same life expectancy in the maternal bloodstream, it is possible to obtain informative results from a KB stain for a fair period of time after a stillbirth. However, if the mother and fetus are ABO incompatible, it is more crucial to quickly perform the KB stain following a stillbirth, as the fetal red blood cells will be eliminated from the maternal bloodstream very quickly, causing the KB stain to underestimate the degree of FMH, if any. Lots of concern has been raised in the literature concerning false positives when sampling is done after delivery. In general this is not a problem. Delivery does result in higher frequency of detection of micro-hemorrhages but this should not confound interpretation of FMH as a possible cause of stillbirth. It is not necessary to draw the sample before induction, onset of labor, delivery, placental delivery etc. despite what some published literature purports. However, if caesarean section is to be used, failure to draw the sample prior to that will result in a 2% false positive rate. Finally, anything which causes persistence of fetal hemoglobin in maternal blood cells will make interpretation much trickier. Certain hemoglobinopathies, the most common of which is sickle cell trait, do this. Overall, somewhere around 1-3% of the time this could result in false interpretation. Breanna Lynn Bartlett-Stewart, stillborn on September 6, 2000 in Paragould, Arkansas to Scott Stewart and Lisa Bartlett, was the first example of a stillbirth whose cause was successfully resolved via the Kleihauer-Betke test[citation needed]. See also
References
|
|
| This article is licensed under the GNU Free Documentation License. It uses material from the Wikipedia article "Kleihauer-Betke_test". A list of authors is available in Wikipedia. |


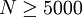 of cells are counted under the microscope and a ratio of fetal to maternal cells generated.
of cells are counted under the microscope and a ratio of fetal to maternal cells generated.



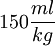
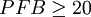 , particularly if the fetus abruptly loses this much blood; in this example, we would hence be likely to suspect FMH as the cause of the stillbirth. It is important to note, however, that such a diagnosis is still not completely conclusive; fetuses losing large quantities of blood over long periods of time are able to compensate for this slower blood loss; since the KB stain tells us nothing with regard to the level of acuity of FMH. This means that it is not possible to entirely correlate a positive KB stain and high
, particularly if the fetus abruptly loses this much blood; in this example, we would hence be likely to suspect FMH as the cause of the stillbirth. It is important to note, however, that such a diagnosis is still not completely conclusive; fetuses losing large quantities of blood over long periods of time are able to compensate for this slower blood loss; since the KB stain tells us nothing with regard to the level of acuity of FMH. This means that it is not possible to entirely correlate a positive KB stain and high 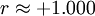 between FMH and stillbirth have been observed.
between FMH and stillbirth have been observed.


