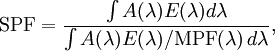To use all functions of this page, please activate cookies in your browser.
my.chemeurope.com
With an accout for my.chemeurope.com you can always see everything at a glance – and you can configure your own website and individual newsletter.
- My watch list
- My saved searches
- My saved topics
- My newsletter
SunscreenSunscreen (also known as sunblock, suntan lotion) is a lotion, spray or other topical product that is supposed to protect the skin from the sun's ultraviolet (UV) radiation, and which reduces sunburn and other skin damage, with the goal of lowering the risk of skin cancer. However, many epidemological studies have shown that the sunscreen-user has a higher risk of skin cancer than the non-user. [1] [2] In Europe and Australia the sunscreen ingredients are not tested by the authorities for photocarcinogenic effects, [3], however, in the USA the newer formulations are tested for photocarcinogenic effects. The most common ingredients in sunscreens on the market today were introduced before this testing became compulsory. In the United States, the term suntan lotion usually means the opposite of sunscreen, and instead refers to lotion designed to moisturize and maximize UV exposure and tanning rather than block it. These are commonly called indoor tanning lotions when designed for use with tanning beds or just suntan lotion if designed for outdoor use and may or may not have SPF protection in them. The most effective sunscreens protect against both UVB (ultraviolet radiation with wavelength between 290 and 320 nanometers), which can cause sunburn, and UVA (between 320 and 400 nanometers), which damages the skin with more long-term effects, such as premature skin aging. Most sunscreens work by containing either an organic chemical compound that absorbs ultraviolet light (such as oxybenzone) or an opaque material that reflects light (such as titanium dioxide, zinc oxide), or a combination of both. Typically, absorptive materials are referred to as chemical blocks, whereas opaque materials are mineral or physical blocks. Product highlight
DosingDosing for sunscreen can be calculated using the formula for body surface area and subsequently subtracting the area covered by clothing that provides effective UV protection. The dose used in FDA sunscreen testing is 2 mg/cm².[4] Provided one assumes an "average" adult build of height 5 ft 4 in (163 cm) and weight 150 lb (68 kg) with a 32 in (82 cm) waist, that adult wearing a bathing suit covering the groin area should apply 29 g (approximately 1 oz) evenly to the uncovered body area. Considering only the face, this translates to about 1/4 to 1/3 of a teaspoon for the average adult face. Contrary to the common advice that sunscreen should be reapplied every 2-3 hours, some research has shown that the best protection is achieved by application 15–30 minutes before exposure, followed by one reapplication 15–30 minutes after the sun exposure begins. Further reapplication is only necessary after activities such as swimming, sweating, and rubbing.[5] However, more recent research at the University of California, Riverside indicates that sunscreen needs to be reapplied within 2 hours in order to remain effective. Not reapplying could even cause more cell damage than not using sunscreen at all, due to the release of extra free radicals from absorbed chemicals.[6] HistoryThe first effective sunscreen may have been developed by chemist Franz Greiter in 1938. The product, called Gletscher Crème (Glacier Cream), subsequently became the basis for the company Piz Buin (named in honor of the place Greiter allegedly obtained the sunburn that inspired his concoction), which today is a well-known marketer of sunscreen products. Some internet articles suggest that Gletscher Crème had a sun protection factor of 2, although a research citation is not readily available online. The first widely used sunscreen was produced by Benjamin Greene, an airman and later a pharmacist, in 1944. The product, Red Vet Pet (for red veterinary petrolatum), had limited effectiveness, working as a physical blocker of ultraviolet radiation. It was a disagreeable red, sticky substance similar to petroleum jelly. This product was developed during the height of World War II, when it was likely that the hazards of sun overexposure were becoming apparent to soldiers in the Pacific and to their families at home. Franz Greiter is credited with introducing the concept of Sun Protection Factor (SPF) in 1962, which has become a worldwide standard for measuring the effectiveness of sunscreen when applied at an even rate of 2 milligrams per square centimeter (mg/cm²). Some controversy exists over the usefulness of SPF measurements, especially whether the 2 mg/cm² application rate is an accurate reflection of people’s actual use. Newer sunscreens have been developed with the ability to withstand contact with water and sweat. Measurements of sunscreen protectionSun protection factorThe SPF of a sunscreen is a laboratory measure of the effectiveness of sunscreen; the higher the SPF, the more protection a sunscreen offers against UV-B (the ultraviolet radiation that causes sunburn). The SPF indicates the time a person can be exposed to sunlight before getting sunburn with a sunscreen applied relative to the time they can be exposed without sunscreen. For example, someone who would burn after 12 minutes in the sun would expect to burn after 2 hours (120 min) if protected by a sunscreen with SPF 10. In practice, the protection from a particular sunscreen depends on factors such as:
The SPF is an imperfect measure of skin damage because invisible damage and skin aging is also caused by the very common ultraviolet type A, which does not cause reddening or pain. Conventional sunscreen does not block UVA as effectively as it does UVB, and an SPF rating of 30+ may translate to significantly lower levels of UVA protection according to a 2003 study. According to a 2004 study, UVA also causes DNA damage to cells deep within the skin, increasing the risk of malignant melanomas.[7] Even some products labeled "broad-spectrum UVA/UVB protection" do not provide good protection against UVA rays.[8] The best UVA protection is provided by products that contain zinc oxide, avobenzone, and ecamsule. Titanium dioxide probably gives good protection, but does not completely cover the entire UV-A spectrum.[9] Due to consumer confusion over the real degree and duration of protection offered, labeling restrictions are in force in several countries. In the United States in 1999, the Food and Drug Administration (FDA) decided to institute the labelling of SPF 30+ for sunscreens offering more protection, and a similar restriction applies in Australia. This was done to discourage companies from making unrealistic claims about the level of protection offered (such as "all day protection"),[10] and because an SPF over 30 does not provide significantly better protection.[citation needed] In the EU sunscreens are limited to SPF 50+, indicating an SPF of 60 or higher.[11]
The SPF can be measured by applying sunscreen to the skin of a volunteer and measuring how long it takes before sunburn occurs when exposed to an artificial sunlight source. In the US, such an in vivo test is required by the FDA. It can also be measured in vitro with the help of a specially designed spectrometer. In this case, the actual transmittance of the sunscreen is measured, along with the degradation of the product due to being exposed to sunlight. In this case, the transmittance of the sunscreen must be measured over all wavelengths in the UV-B range (290–350 nm), along with a table of how effective various wavelengths are in causing sunburn (the erythemal action spectrum) and the actual intensity spectrum of sunlight (see the figure). Such in vitro measurements agree very well with in vivo measurements.[12] Mathematically, the SPF is calculated from measured data as where E(λ) is the solar irradiance spectrum, A(λ) the erythemal action spectrum, and MPF(λ) the monochromatic protection factor, all functions of the wavelength λ. The MPF is roughly the inverse of the transmittance at a given wavelength. The above means that the SPF is not simply the inverse of the transmittance in the UV-B region. If that were true, then applying two layers of SPF 5 sunscreen would be equivalent to SPF 25 (5 times 5). The actual combined SPF is always lower than the square of the single-layer SPF. Measurements of UVA protectionPersistent Pigment Darkening (PPD), Immediate Pigment Darkening (IPD), Boots Star System, Japanese PA system
The PPD is used as part of guidelines for EU sunscreens to provide the consumer with a minimum of UVA protection in relation to the SPF. The PPD should be at least 1/3 of the SPF to carry the UVA seal. The implementation of this seal is in its phase-in period, so a sunscreen without may already offer this protection. [13] The Japanese PA system ranges from PA+ to PA+++, with the + sign indicating increased UVA protection. However, studies have found the PA system to be inadequate, since the maximum PA (PA+++) is equivalent to a minimum protection of PPD8. Star rating systemIn the UK and Ireland, a star rating system is used to describe the ratio of UVA to UVB protection offered by sun screen creams and sprays. Invented by Dr Diffey of the Boots Company in Nottingham UK, it has been adopted by most companies marketing these products in the UK. It should not be confused with SPF which is measured with reference to burning and UVB. One star products provide the least ratio of UVA protection, five star products are the best. Active ingredientsThe principal ingredients in sunscreens are usually aromatic molecules conjugated with carbonyl groups. This general structure allows the molecule to absorb high-energy ultraviolet rays and release the energy as lower-energy rays, thereby preventing the skin-damaging ultraviolet rays from reaching the skin. So, upon exposure to UV light, most of the ingredients (with the notable exception of avobenzone) do not undergo significant chemical change, allowing these ingredients to retain the UV-absorbing potency without significant photo-degradation.[4] The following are the FDA allowable active ingredients in sunscreens:
Recently FDA approved:
Others approved within the EU[14] and other parts of the world[15] include:
A lot of the ingredients not approved by the FDA are relatively new and developed to absorb UVA.[16] MelaninThe hormone alpha-melanocyte stimulating hormone is made when the body is exposed to sunlight and is responsible for the development of the pigment melanin. Research is being done to create stable artificial forms of the hormone. A promising candidate, melanotan, might be useful in the prevention of skin cancer, by causing tanning without the need for exposure to dangerous levels of UV. Possible adverse effectsSome individuals can have mild to moderate allergic reactions to certain ingredients in sunscreen, particularly the chemical benzophenone, which is also known as phenyl ketone, diphenyl ketone, or benzoylbenzene. It is not clear how much of benzophenone is absorbed into the bloodstream, but trace amounts can be found in urinalysis after use. Sunscreens are effective in reducing sunburn, but not necessarily the risk of cancer. A study published in April 1992, entitled "Could sunscreens increase melanoma risk?" reported that the greatest increase in melanoma occurred in those regions where sunscreen use is most prevalent.[17] The authors point out that "the SPF of sunscreens concerns solely their ability to absorb ultraviolet B (UV-B) light. Even sunscreens with high SPF factors can be completely transparent to ultraviolet A (UV-A), which includes 90 to 95% of ultraviolet light. UV-A blocking ingredients, which have commonly been added to most sunscreens since 1989, block only half the UV-A spectrum and provide a protection factor against delayed UV-A induced erythema of only 1.7 at usual concentrations. Both UV-A and UV-B have been shown to mutate DNA and promote skin cancers in animals. UV-A also penetrates deeper into the skin than UV-B... two studies suggest that sunscreens may not be effective in preventing skin cancer. A large case-control study showed higher risks of melanoma in men who used sunscreens, and a large prospective study showed a higher incidence of basal cell carcinoma in women who used sunscreens." Recently, there has been increased attention to the possibility of adverse health effects associated with the synthetic compounds in most sunscreens.[18] Recent studies found that some sunscreens generate harmful compounds that might promote skin cancer. The three commonly used ultraviolet (UV) filters -- octylmethoxycinnamate, benzophenone 3, and octocrylene -- eventually soak into the deeper layers of the skin after their application, leaving the top skin layers vulnerable to sun damage. UV rays absorbed by the skin can generate harmful compounds called reactive oxygen species (ROS), which can cause skin cancer and premature aging. The researchers found that once the filters in sunscreen soak into the lower layers of skin, the filters react with UV light to create more damaging ROS.[6] To reduce ROS generation and damage, the researchers recommend reapplying the sunscreen often, which will replenish the sunscreen which has penetrated the skin. Future possibilities may include the development of sunscreens which stay at the surface of the skin, or mixing sunscreens with antioxidants that can neutralize ROS.[19] A significant reduction in sun exposure inhibits the production of vitamin D. The use of sunscreen with a sun protection factor (SPF) of 8 inhibits more than 95% of vitamin D production in the skin.[20] However, excessive sun exposure has been conclusively linked to some forms of skin cancer and signs of premature aging. Season, geographic latitude, time of day, cloud cover, smog, skin type, and sunscreen all have an effect on vitamin D production in the skin.[21] Fifteen minutes per day of direct exposure to the sun (i.e. without sunscreen) is a generally accepted guideline to follow for optimum vitamin D production.[22] References
See also
Categories: Dermatological preparations | Sunscreening agents |
|
| This article is licensed under the GNU Free Documentation License. It uses material from the Wikipedia article "Sunscreen". A list of authors is available in Wikipedia. |